|
Overview
 A normal foot should arch so the middle of the foot does not touch the ground when the patient stands up. If it does touch, the patient has a flat foot or fallen arch. Flat feet are normal for young children. Their arches should develop by adulthood, but sometimes they fail to develop. Some people with flat feet have pain in the heel or arch, but others do not. Causes Over-pronation is a common biomechanical problem that occurs when the arches collapse while walking or standing. This condition hampers our natural walking pattern, causing an imbalance, and leading to wear and tear in other parts of the body with every step we take. Whether you suffer from over-pronation like most of the population, or you have a true flat foot, in both cases your poor walking pattern may contribute to a range of different complaints. As we age, poor aligment of the feet causes very common conditions such as heel pain or knee pain. Over-pronation has different causes. Obesity, pregnancy, age or repetitive pounding on a hard surface can weaken the arch, leading to over-pronation. Over-pronation is also very common with athletes, especially runners, who most of them nowadays use orthotics inside their shoes. Symptoms Arches can be seen as ?rolling downward? or collapsing when walking. Pain may present in lower back, hips or knees. Pain may be present on the bottom of the heels, within the arch, within the ankles or even the forefoot. Swelling can occur. Pain may occur in the anterior leg muscles. Diagnosis People who have flat feet without signs or symptoms that bother them do not generally have to see a doctor or podiatrist about them. However, if any of the following occur, you should see your GP or a podiatrist. The fallen arches (flat feet) have developed recently. You experience pain in your feet, ankles or lower limbs. Your unpleasant symptoms do not improve with supportive, well-fitted shoes. Either or both feet are becoming flatter. Your feet feel rigid (stiff). Your feet feel heavy and unwieldy. Most qualified health care professionals can diagnose flat feet just by watching the patient stand, walk and examining his/her feet. A doctor will also look at the patient's medical history. The feet will be observed from the front and back. The patient may be asked to stand on tip-toe while the doctor examines the shape and functioning of each foot. In some cases the physician may order an X-ray, CT (computed tomography) scan, or MRI (magnetic resonance imaging) scan. What does it mean when you have flat feet? Non Surgical Treatment Traditionally, running shoes have contained extra padding to support the feet in general and fallen arches in particular. Orthopedists may prescribe orthotics for people with flat feet. More recently, however, the argument has arisen for shoes that provide a more minimal amount of padding and support for the feet. The idea here is that the feet will strengthen themselves. Since there are multiple options, anyone with flat feet or fallen arches would do well to explore them all. Surgical Treatment  Feet that do not respond to the treatments above may need surgery. The surgery will help to create a supportive arch. After Care Patients may go home the day of surgery or they may require an overnight hospital stay. The leg will be placed in a splint or cast and should be kept elevated for the first two weeks. At that point, sutures are removed. A new cast or a removable boot is then placed. It is important that patients do not put any weight on the corrected foot for six to eight weeks following the operation. Patients may begin bearing weight at eight weeks and usually progress to full weightbearing by 10 to 12 weeks. For some patients, weightbearing requires additional time. After 12 weeks, patients commonly can transition to wearing a shoe. Inserts and ankle braces are often used. Physical therapy may be recommended. There are complications that relate to surgery in general. These include the risks associated with anesthesia, infection, damage to nerves and blood vessels, and bleeding or blood clots. Complications following flatfoot surgery may include wound breakdown or nonunion (incomplete healing of the bones). These complications often can be prevented with proper wound care and rehabilitation. Occasionally, patients may notice some discomfort due to prominent hardware. Removal of hardware can be done at a later time if this is an issue. The overall complication rates for flatfoot surgery are low.
0 Comments
Overview
 Heel pain can be very aggravating, especially when taking those first steps in the morning. The key to decreasing and possibly eliminating heel pain is to stretch your heel cord and plantar fascia. The heel cord is the Achilles tendon, which connects the gastrocnemius and soleus muscles in the calf to the heel bone. The plantar fascia is a thick tissue that runs along the bottom of your foot, connecting the heel bone to the toes and maintaining the arch. Causes In the majority of cases, heel pain has a mechanical cause. It may also be caused by arthritis, infection, an autoimmune problem trauma, a neurological problem, or some other systemic condition (condition that affects the whole body). Symptoms Initially, this pain may only be present when first standing up after sleeping or sitting. As you walk around, the muscle and tendon loosen and the pain goes away. As this problem progresses, the pain can be present with all standing and walking. You may notice a knot or bump on the back of the heel. Swelling may develop. In some cases, pressure from the back of the shoe causes pain. Diagnosis Your doctor will perform a physical exam and ask questions about your medical history and symptoms, such as have you had this type of heel pain before? When did your pain begin? Do you have pain upon your first steps in the morning or after your first steps after rest? Is the pain dull and aching or sharp and stabbing? Is it worse after exercise? Is it worse when standing? Did you fall or twist your ankle recently? Are you a runner? If so, how far and how often do you run? Do you walk or stand for long periods of time? What kind of shoes do you wear? Do you have any other symptoms? Your doctor may order a foot x-ray. You may need to see a physical therapist to learn exercises to stretch and strengthen your foot. Your doctor may recommend a night splint to help stretch your foot. Surgery may be recommended in some cases. Non Surgical Treatment If you still have pain after several weeks, see your foot and ankle surgeon, who may add one or more of these treatment approaches, padding and strapping. Placing pads in the shoe softens the impact of walking. Strapping helps support the foot and reduce strain on the fascia. Orthotic devices. Custom orthotic devices that fit into your shoe help correct the underlying structural abnormalities causing the plantar fasciitis. Injection therapy. In some cases, corticosteroid injections are used to help reduce the inflammation and relieve pain. Removable walking cast. A removable walking cast may be used to keep your foot immobile for a few weeks to allow it to rest and heal. Night splint. Wearing a night splint allows you to maintain an extended stretch of the plantar fascia while sleeping. This may help reduce the morning pain experienced by some patients. Physical therapy. Exercises and other physical therapy measures may be used to help provide relief. Surgical Treatment If treatment hasn't worked and you still have painful symptoms after a year, your GP may refer you to either an orthopaedic surgeon, a surgeon who specialises in surgery that involves bones, muscles and joints or a podiatric surgeon, a podiatrist who specialises in foot surgery. Surgery is sometimes recommended for professional athletes and other sportspeople whose heel pain is adversely affecting their career. Plantar release surgery is the most widely used type of surgery for heel pain. The surgeon will cut the fascia to release it from your heel bone and reduce the tension in your plantar fascia. This should reduce any inflammation and relieve your painful symptoms. Surgery can be performed either as open surgery, where the section of the plantar fascia is released by making a cut into your heel or endoscopic or minimal incision surgery - where a smaller incision is made and special instruments are inserted through the incision to gain access to the plantar fascia. Endoscopic or minimal incision surgery has a quicker recovery time, so you will be able to walk normally much sooner (almost immediately), compared with two to three weeks for open surgery. A disadvantage of endoscopic surgery is that it requires both a specially trained surgical team and specialised equipment, so you may have to wait longer for treatment than if you were to choose open surgery. Endoscopic surgery also carries a higher risk of damaging nearby nerves, which could result in symptoms such as numbness, tingling or some loss of movement in your foot. As with all surgery, plantar release carries the risk of causing complications such as infection, nerve damage and a worsening of your symptoms after surgery (although this is rare). You should discuss the advantages and disadvantages of both techniques with your surgical team. deelsonheels Prevention  You should always wear footwear that is appropriate for your environment and day-to-day activities. Wearing high heels when you go out in the evening is unlikely to be harmful. However, wearing them all week at work may damage your feet, particularly if your job involves a lot of walking or standing. Ideally, you should wear shoes with laces and a low to moderate heel that supports and cushions your arches and heels. Avoid wearing shoes with no heels. Do not walk barefoot on hard ground, particularly while on holiday. Many cases of heel pain occur when a person protects their feet for 50 weeks of the year and then suddenly walks barefoot while on holiday. Their feet are not accustomed to the extra pressure, which causes heel pain. If you do a physical activity, such as running or another form of exercise that places additional strain on your feet, you should replace your sports shoes regularly. Most experts recommend that sports shoes should be replaced after you have done about 500 miles in them. It is also a good idea to always stretch after exercising, and to make strength and flexibility training a part of your regular exercise routine. Overview
Epiphysiodesis is a surgical option designed to slow down the growth of the long leg over a period of months to years. It is only used in growing children. The operation involves a general anaesthetic. Small incisions are made around the knee near the growth plates of the thigh bone and the shin bone. The growth plates are prevented from growing by the use of small screws and plates (?8 - plates?). The screws are buried beneath the skin and are not visible. Stitches are buried beneath the skin and do not need to be removed. The child is normally in hospital for 2-3 days. The child can weight bear immediately and return back to normal activity within a few weeks. Long term follow up is required to monitor the effects of the surgery. The timing of the surgery is based on the amount of growth predicted for the child. Therefore, this procedure can under- and over-correct the difference in leg length. Occasionally the screws have to be removed to allow growth to continue. This procedure can be used on one half of the growth plate to correct deformity in a limb e.g. knock-knees or bow legs. This is known as hemiepiphysiodesis.  Causes Some limb-length differences are caused by actual anatomic differences from one side to the other (referred to as structural causes). The femur is longer (or shorter) or the cartilage between the femur and tibia is thicker (or thinner) on one side. There could be actual deformities in one femur or hip joint contributing to leg length differences from side to side. Even a small structural difference can amount to significant changes in the anatomy of the limb. A past history of leg fracture, developmental hip dysplasia, slipped capital femoral epiphysis (SCFE), short neck of the femur, or coxa vara can also lead to placement of the femoral head in the hip socket that is offset. The end-result can be a limb-length difference and early degenerative arthritis of the hip. Symptoms LLD do not have any pain or discomfort directly associated with the difference of one leg over the other leg. However, LLD will place stress on joints throughout the skeletal structure of the body and create discomfort as a byproduct of the LLD. Just as it is normal for your feet to vary slightly in size, a mild difference in leg length is normal, too. A more pronounced LLD, however, can create abnormalities when walking or running and adversely affect healthy balance and posture. Symptoms include a slight limp. Walking can even become stressful, requiring more effort and energy. Sometimes knee pain, hip pain and lower back pain develop. Foot mechanics are also affected causing a variety of complications in the foot, not the least, over pronating, metatarsalgia, bunions, hammer toes, instep pain, posterior tibial tendonitis, and many more. Diagnosis The doctor carefully examines the child. He or she checks to be sure the legs are actually different lengths. This is because problems with the hip (such as a loose joint) or back (scoliosis) can make the child appear to have one shorter leg, even though the legs are the same length. An X-ray of the child?s legs is taken. During the X-ray, a long ruler is put in the image so an accurate measurement of each leg bone can be taken. If an underlying cause of the discrepancy is suspected, tests are done to rule it out. Non Surgical Treatment In an adult, we find that we can add a non compressive silicone heel lift to a shoe in increments of 3-4 mm maximum per week. Were we to give a patient with a 20 mm short leg, 20 mm of lift all at once, their entire body would rebel. The various compensations that the body has made, such as curvatures and shortening of muscles on the convex side of the curve, would make such a dramatic change not just noticeable, but painful. When we get close to balancing a patient by lifting a leg with heel inserts, then we perform another gait analysis and follow up xray. At that point, we can typically write them a final prescription to have their shoe modified. A heel lift is typically fine up to 7 mm. When it gets higher than that, the entire shoe must be modified. There are two reasons for this. The back of the shoe is generally too short to accommodate more than 7-8 mm inserted inside the shoes and a heel lift greater than 7 mm will lead to Achilles tendon shortening, which then creates it?s own panoply of problems.  what is a shoe lift? Surgical Treatment Many people undergo surgery for various reasons - arthritis, knee replacement, hip replacement, even back surgery. However, the underlying cause of leg length inequality still remains. So after expensive and painful surgery, follow by time-consuming and painful rehab, the true culprit still remains. Resuming normal activities only continues to place undue stress on the already overloaded side. Sadly so, years down the road more surgeries are recommended for other joints that now endure the excessive forces. Overview
 People think of a bunion as being as a bump on the side of the foot near the big toe. However, bunions go deeper than what we can see. Although the skin might be red, a bunion actually reflects a change in the anatomy of the foot. Bunions happen over time. What begins as the big toe pointing toward the second toe ends up as changes in the actual alignment of the bones in the foot. There is also a condition called tailor?s bunion or bunionette. This type of bump differs from a bunion in terms of the location. A tailor?s bunion is found near the base of the little toe on the outside of the foot. Causes Bunions form when the normal balance of forces exerted on the joints and tendons of your feet are disrupted. This can lead to instability in the big toe joint - also known as the first metatarsophalangeal (MTP) joint, causing a deformity. Bunions develop over years of abnormal motion and pressure on your big toe joint. They often result from a combination of your inherited foot type, faulty foot mechanics that affect the way you walk and shoes that fit improperly. Other causes of bunions include foot injuries. Deformities present at birth (congenital). Neuromuscular disorders, such as cerebral palsy or post- polio syndrome (post-poliomyelitis). Bunions may be associated with various forms of arthritis, including inflammatory or degenerative, causing the protective cartilage that covers your big toe joint to deteriorate. An occupation that puts extra stress on your feet also can be a cause. Waiters, factory workers, dancers and athletes often are more prone to developing bunions. SymptomsA bunion, also called a hallux valgus, is a bony prominence on the inside of the big toe, caused by a misalignment of the joint. The overlying skin maybe swollen, red and tender. Bunions are often painful and can limit what shoes you can wear. Diagnosis People with bunions may be concerned about the changing appearance of their feet, but it is usually the pain caused by the condition that leads them to consult their doctor. The doctor will evaluate any symptoms experienced and examine the affected foot for joint enlargement, tissue swelling and/or tenderness. They will also assess any risk factors for the condition and will ask about family history. An x-ray of the foot is usually recommended so that the alignment of big toe joint can be assessed. This would also allow any other conditions that may be affecting the joint, such as arthritis, to be seen. Non Surgical Treatment There is no way to eliminate existing bunions except to have them surgically removed. There are nonsurgical measures you can take to alleviate the pain and prevent your bunions from increasing in severity, and for that reason it's important to see your doctor before they become a serious problem. The more extensive your bunions are, the less effective nonsurgical treatments are. On the other hand, most bunions can be dealt with without surgery through wearing roomier, low-heel shoes, padding and taping your feet, using medications for pain control, going to physical therapy to relieve inflammation and wearing orthotics in your shoes to correct mechanical problems. Bunions that are not causing pain generally aren't appropriate for surgery. Roomier shoes. You should seek out shoes that conform to the shape of your feet as much as possible and provide plenty of room in the toe box, ensuring that your toes are not pinched or squeezed. You should make sure that, while standing, there is a half inch of space for your longest toe at the end of each shoe. Make sure the ball of your foot fits comfortably in the widest part of the shoe. Feet normally swell during the course of the day, so shop for shoes at the end of the day, when your feet are at their largest. Don't be vain about your shoe size, sizes vary by brand, so concentrate on making certain your shoes are comfortable. Remember that your two feet are very likely to be different sizes and fit your shoe size to the larger foot. Low-heel shoes. High heels shift all your body weight onto your toes, increasing the pressure on your toes and their joints tremendously. Instead, wear shoes with low (less than two inches) or flat heels that fit your foot comfortably. Padding and Taping. Padding the bunion can minimize pain and allow you to walk more normally. Specially designed pads for this are available at most drugstores. Taping your foot can reduce stress and pain in it by helping it stay in a more normal position. Medication. Anti-inflammatory drugs such as aspirin and ibuprofen can help deal with pain and inflammation caused by your bunion. Cortisone injections may be prescribed for the same purpose. If your bunion is a consequence of arthritis in the MTP joint, your physician may prescribe medications for that. Physical Therapy. Ultrasound treatments and whirlpool baths can help reduce pain and inflammation in bunions and related tissues. Orthotics are shoe inserts that can help correct mechanical foot-motion problems to reduce pain and prevent worsening of your bunion. Other measures. Icing and elevating your foot when your bunion is painful may help. Having your shoes stretched at a shoe repair shop may help also.  Surgical Treatment Surgical treatment for bunion deformities usually involves an osteotomy, a procedure in which a cut or cuts are made in the affected bone or bones to restore proper alignment. Different techniques are used depending on the type of deformity; selection is guided by the degree of deformity present and the goals of preventing recurrence and achieving the most rapid recovery possible. Some of the more common procedures are. The distal chevron osteotomy: a procedure in which a v-shaped cut is made at the toe end of the first metatarsal. This surgery is appropriate for individuals who have a congruent deformity, one in which there is a painful prominence at the base of the toe, but the joint is still well aligned. Absorbable pins are placed in the metatarsal to maintain alignment during healing. The Scarf or Ludloff osteotomy: in this procedure, a more extensive cut is made higher up in the metatarsal to correct a moderate incongruent deformity and metatarsus primus varus. Screws are used to maintain alignment during healing. The crescent osteotomy: a procedure in which a curved cut is made at the base of the metatarsal is appropriate for patients with more severe metatarsus primus varus and, therefore, require more correction. Screws or pins are used to maintain alignment. The Lapidus procedure: individuals who have severe deformity, instability of the first ray, with a loose metatarsal-tarsal joint (located in the mid-foot) may not get enough correction from an osteotomy alone. Moreover, the looseness of the joint may lead to recurrence or be causing pain on the ball of the foot because the first metatarsal is floating up, allowing for excessive weight to go to adjacent metatarsals (commonly the second and the third). In such cases, the metatarsal-tarsus joint is fused to provide lasting stability. Screws are used to maintain alignment. The loss of motion from the fusion is small and does not significantly limit motion of the big toe. Patients undergoing bunion surgery are given an ankle block that anesthetizes the foot from the ankle down. Depending on individual preference, a sedative may be given as well and the patient can be as sedated as they wish. All bunion surgeries may be done on a same-day basis, eliminating the need for hospitalization. Overview
 A bunion is an abnormal bump, or bony enlargement that forms at the base of your big toe. In the early stages, the bunion may be small and the side of your foot may be slightly swollen. As it progresses, the bump gets larger and becomes increasingly painful. Your big toe may point towards your other toes, rather than straight. Shoes may be uncomfortable to wear and add to the irritation of the joint. Causes Bunions occur with greater regularity in women than men, and they may sometimes run in families. You may also have an increased likelihood of bunions if you are born with certain bone abnormalities in your feet. Factors that may increase your chances of developing a bunion include long-term use of narrow-toed and/or high-heeled footwear. Arthritis. Toe trauma. Laxity of your connective tissues (ligament laxity). Limb length inequalities. Genetics. Certain foot problems (e.g. flatfoot, over-pronation, etc.). SymptomsWith an advanced bunion, the big toe joint can be significantly deformed. The big toe can crowd the other toes and may lie over or under the second toe. The larger the bunion gets, the more it hurts to walk. Wearing any type of shoe can be painful. Symptoms of bunions tend to increase over time as the condition worsens. Typical symptoms include deformity of the big toe joint. Growth of a bony lump (exostosis) at the side of the big toe joint. Pain, redness and tissue swelling (bursitis) over the big toe joint, with thickening of overlying skin. Pain when walking (particularly during the "push off" phase). Overlapping of the big toe above or below the second toe in severe cases. Diagnosis People with bunions may be concerned about the changing appearance of their feet, but it is usually the pain caused by the condition that leads them to consult their doctor. The doctor will evaluate any symptoms experienced and examine the affected foot for joint enlargement, tissue swelling and/or tenderness. They will also assess any risk factors for the condition and will ask about family history. An x-ray of the foot is usually recommended so that the alignment of big toe joint can be assessed. This would also allow any other conditions that may be affecting the joint, such as arthritis, to be seen. Non Surgical Treatment Patients who suffer from bunions are usually referred to a surgeon. Unfortunately, surgery often makes the problem worse. Surgeons will use x-ray technology as a diagnostic tool, which does not always properly diagnose the pain source. Another problem with this approach is that it does not do anything to strengthen the weakened ligament in the foot and, thus, does not alleviate the chronic pain that people with this condition experience. Another standard practice of modern medicine is to use steroids or to prescribe anti-inflammatory medications. However, in the long run, these treatments do more damage than good. Cortisone shots and anti-inflammatory drugs have been shown to produce short-term pain benefit, but both result in long-term loss of function and even more chronic pain by actually inhibiting the healing process of soft tissues and accelerating cartilage degeneration. Plus, long-term use of these drugs can lead to other sources of chronic pain, allergies and leaky gut syndrome. 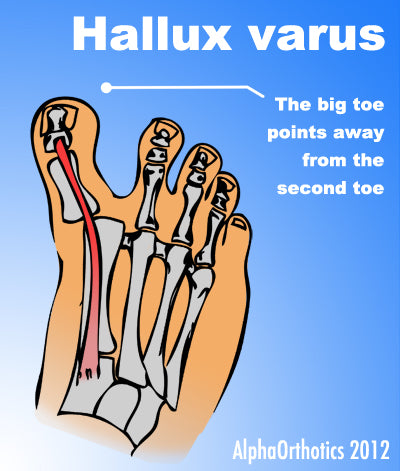 Surgical Treatment Bunionectomy is a general term that describes a variety of bone and soft tissue procedures that are intended to realign your big toe and reduce the prominence at the base of your big toe. The procedures chosen are based on numerous factors, including measured angular displacement of your involved joints (especially your first MTP joint). The degree of pain you are experiencing. The degree of joint dislocation and cartilage damage within your affected joint. Flexibility of your adjacent joints. Flexibility of soft tissues in your problem area. Overview
 The term ?bunion,? as it is popularly used, describes a variety of deformities involving a painful prominence and swelling at the base of the big toe. Orthopaedists use additional terms to describe the different deformities. The condition in which the big toe deviates from the normal position toward the direction of the second toe is referred to as hallux valgus. Dorsal bunions are a different variety in which the prominence appears on the top of the base of the toe, often the result of an arthritic joint. Causes No single cause or set of causes for bunions has been identified, although gender-women develop them more frequently than men-and heredity play a role. In addition, the foot gradually widens with age as the ligaments that connect the bones in the forefoot become more lax. Contrary to what many people believe, ill-fitting footwear is not the cause of bunions. In fact, bunions are found in populations all over the world, including among those who never wear shoes. Shoes that are too tight can, however, contribute to the progression of the condition. Bunions are often bilateral, that is, appearing in both feet. Although bunions are usually seen in people who are middle-aged or older, there are adolescents who are diagnosed with the condition, usually the result of a congenital problem. SymptomsThe most obvious symptoms of a bunion are. Pain in the area of the MTP joint, the joint where your big toe connects to your foot. Bending of the big toe in towards the other toes. An enlarged bump of bone or tissue at the MTP joint. Each symptom can range in degree from small to severe. Sometimes the pain can be sufficient to make it difficult to walk in normal shoes. Other symptoms may include. Swelling and inflammation of the skin around the MTP joint. Thickening of the skin in the area of the joint. Restricted motion in your big toe. Pressure from the inward bending of your big toe can affect your other toes, leading to corns on your smaller toes. Ingrown toenails on the smaller toes. Development of hammertoes in the other toes. Calluses on the bottom of your foot. If you have any of these symptoms, especially pain, displacement of your big toe or development of a bulge, you should consider consulting your physician. Even if you're not significantly bothered by some of these symptoms, bunions tend to continue getting bigger and more serious over time and should be taken care of before they do so. Diagnosis Clinical findings are usually specific. Acute circumferential intense pain, warmth, swelling, and redness suggest gouty arthritis (see Gout) or infectious arthritis (see Acute Infectious Arthritis), sometimes mandating examination of synovial fluid. If multiple joints are affected, gout or another systemic rheumatic disease should be considered. If clinical diagnosis of osteoarthritic synovitis is equivocal, x-rays are taken. Suggestive findings include joint space narrowing and bony spurs extending from the metatarsal head or sometimes from the base of the proximal phalanx. Periarticular erosions (Martel sign) seen on imaging studies suggest gout. Non Surgical Treatment Nonsurgical treatments that may relieve the pain and pressure of a bunion include changing shoes. Wear roomy, comfortable shoes that provide plenty of space for your toes. Padding and taping or splinting. Your doctor can help you tape and pad your foot in a normal position. This can reduce stress on the bunion and alleviate your pain. Medications. Acetaminophen (Tylenol, others), ibuprofen (Advil, Motrin IB, others) or naproxen (Aleve) can help you control the pain of a bunion. Cortisone injections also can be helpful. Shoe inserts. Padded shoe inserts can help distribute pressure evenly when you move your feet, reducing your symptoms and preventing your bunion from getting worse. Over-the-counter arch supports can provide relief for some people, although others may require prescription orthotic devices. Applying ice. Icing your bunion after you've been on your feet too long can help relieve soreness and inflammation. Surgical Treatment In severe hallux valgus bunion cases, the first long bone (metatarsal) in the foot dramatically shifts away from the second metatarsal, resulting in looseness and a large deformity. In severe bunion corrections, a surgery known as the Lapidus procedure realigns the first metatarsal into its natural position. Using screws, the surgery holds the bone stable so it does not shift again and reduces the change of the bunion returning to basically none. Surgery may also involve removing the enlarged portion of the bunion region, cutting and realigning the bone, and correcting the position of the tendons and ligaments. By using a special plate with Lapidus procedures, University Foot and Ankle Institute patients are able to put weight on their foot after only 2-3 weeks, rather than the typical 6-8 weeks of no weight.
Overview
 A bunion or hallux valgus is a prominence on the inner border of the foot effecting the big toe and at the level of the 1st metatarso-phalangeal (MTP) joint. The bunion prominence which is seen and felt on the inner border of the foot is not due to any growth of bone but is due to the 1st metatarsal bone. With a bunion this has become more prominent than normal because the 1st metatarsal has moved away from its immediate neighbour the 2nd metatarsal. This widens the forefoot thus producing the bunion. An inevitability of the splaying of the foot which occurs with a bunion or hallux valgus is that the great toe itself is then pulled across in the opposite direction (towards the second toe) by the still normally located tendons of the big toe. A bunion or hallux valgus is commonly confused with hallux interphalangeus (where the deformity lies more distally and which tends to be less problematic). Here there is no increase in the space between the metatarsals, and the deformity lies in the shape of the phalynx bone. Causes Bunions form when the normal balance of forces that is exerted on the joints and tendons of the foot becomes disrupted. This disruption can lead to instability in the joint and cause the deformity. Bunions are brought about by years of abnormal motion and pressure over the MTP joint. They are, therefore, a symptom of faulty foot development and are usually caused by the way we walk and our inherited foot type or our shoes. SymptomsThe most common complaint with bunions is pain that develops over the large bump due to shoe pressure. A red, inflamed area can develop, called a bursa. With ongoing pressure, the inflammation can cause throbbing, as it presses against the blood vessels, or swelling in the joint. Shooting pains occur when the swelling presses against the nerve. If left untreated, the constant irritation can lead to arthritis that breaks down the joint, resulting in pain and stiffness. Diagnosis Most patients are diagnosed to have bunions from clinical history and examination. However, in some cases, X-rays will be performed to determine the extent of damage to the joint. Furthermore, it will enable the treating doctor to decide on the best course of management of the patient. Non Surgical Treatment Treatment options are based on the severity of the deformity and symptoms. Nonsurgical treatments usually are enough to relieve the pain and pressure on the big toe. Your doctor may tell you to start wearing roomy, comfortable shoes and use toe padding or a special corrective device that slips into your shoes to push the big toe back into its proper position. To help relieve pain, you can take over-the-counter medications such as acetaminophen (Tylenol) or ibuprofen (Advil, Motrin and others). Whirlpool baths also may help to ease discomfort. A bunion or hallux valgus is a prominence on the inner border of the foot effecting the big toe and at the level of the 1st metatarso-phalangeal (MTP) joint. The bunion prominence which is seen and felt on the inner border of the foot is not due to any growth of bone but is due to the 1st metatarsal bone. With a bunion this has become more prominent than normal because the 1st metatarsal has moved away from its immediate neighbour the 2nd metatarsal. This widens the forefoot thus producing the bunion. An inevitability of the splaying of the foot which occurs with a bunion or hallux valgus is that the great toe itself is then pulled across in the opposite direction (towards the second toe) by the still normally located tendons of the big toe. A bunion or hallux valgus is commonly confused with hallux interphalangeus (where the deformity lies more distally and which tends to be less problematic). Here there is no increase in the space between the metatarsals, and the deformity lies in the shape of the phalynx bone. Causes Bunions form when the normal balance of forces that is exerted on the joints and tendons of the foot becomes disrupted. This disruption can lead to instability in the joint and cause the deformity. Bunions are brought about by years of abnormal motion and pressure over the MTP joint. They are, therefore, a symptom of faulty foot development and are usually caused by the way we walk and our inherited foot type or our shoes. SymptomsThe most common complaint with bunions is pain that develops over the large bump due to shoe pressure. A red, inflamed area can develop, called a bursa. With ongoing pressure, the inflammation can cause throbbing, as it presses against the blood vessels, or swelling in the joint. Shooting pains occur when the swelling presses against the nerve. If left untreated, the constant irritation can lead to arthritis that breaks down the joint, resulting in pain and stiffness. Diagnosis Most patients are diagnosed to have bunions from clinical history and examination. However, in some cases, X-rays will be performed to determine the extent of damage to the joint. Furthermore, it will enable the treating doctor to decide on the best course of management of the patient. Non Surgical Treatment Treatment options are based on the severity of the deformity and symptoms. Nonsurgical treatments usually are enough to relieve the pain and pressure on the big toe. Your doctor may tell you to start wearing roomy, comfortable shoes and use toe padding or a special corrective device that slips into your shoes to push the big toe back into its proper position. To help relieve pain, you can take over-the-counter medications such as acetaminophen (Tylenol) or ibuprofen (Advil, Motrin and others). Whirlpool baths also may help to ease discomfort. 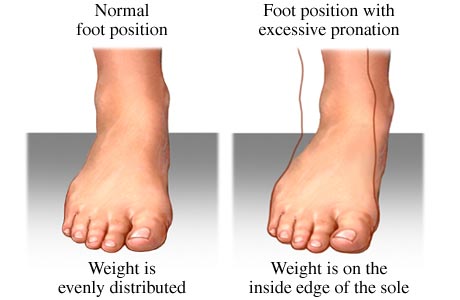 Surgical Treatment According to the NHS, 85 per cent of operations are successful, but there?s no guarantee that the problem won?t recur, that the pain will go away, or that your movement won?t become limited. Ask yourself if the affront to your vanity and discomfort caused by your bunion is worth the post-op suffering, and if you can cope with the inevitable restriction on your movement that means no driving and time off work, even if only for a few weeks. Surgical Treatment According to the NHS, 85 per cent of operations are successful, but there?s no guarantee that the problem won?t recur, that the pain will go away, or that your movement won?t become limited. Ask yourself if the affront to your vanity and discomfort caused by your bunion is worth the post-op suffering, and if you can cope with the inevitable restriction on your movement that means no driving and time off work, even if only for a few weeks.
|
AuthorWrite something about yourself. No need to be fancy, just an overview. Archives
July 2017
Categories |
 RSS Feed
RSS Feed
